
In France, an epidural is the most common way to reduce, or even eliminate, the pain of contractions and the baby’s passage during childbirth while allowing you to remain mobile and awake. Its use became widespread in the 1990s: today, 82.6% of women in France use it (according to the 2016 National Perinatal Survey).
And yet, the epidural needle can be intimidating. The reason for this discomfort: its size. We explain everything!
How big is the epidural needle?
Let’s start right away with the uncomfortable question: exactly how big is this famous epidural needle? The answer is… 80 mm (that is, 8 centimeters)!
That said, for most women, the needle is not inserted all the way (sometimes not even halfway!). In fact, the epidural needle is that long to ensure it can reach the epidural space regardless of the patient’s body type.
As for its diameter, the needle measures 1.3 mm. This is because it must allow insertion of the catheter (a small plastic tube used to administer the anesthetics).
What are the steps involved in administering an epidural?
First of all, whether or not you choose to have an epidural during labor, you should know that you will still need to attend the mandatory consultation during the 8th month with the anesthesiologist to go over all possibilities. This does not force you to say yes to an epidural! But it is a chance to ask all your questions.
During this consultation, the anesthesiologist will ask about your medical history, allergies, and any current treatments. They will also perform a clinical examination. In particular, if you want an epidural, the anesthesiologist will examine your back (where the epidural will be placed during labor).
So, how is the epidural needle actually inserted on the big day?
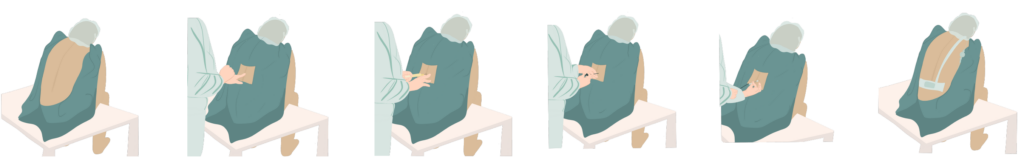
- 1 – First, you will be seated on the bed: bare back, sitting cross-legged or with your legs dangling, wearing a surgical cap, and asked to curve your back, lowering your head and shoulders as if you were carrying something very heavy.
- 2 – The anesthesiologist disinfects the skin, places a sterile drape on your back, and locates their landmarks by feeling your back. From that point on, care must be taken not to touch that area anymore, because it must remain clean.
- 3 – The anesthesiologist performs a local anesthetic on the skin with a small needle, just like at the dentist’s office.
- 4 – After waiting for the local anesthetic to take effect (between 1 and 2 minutes), they insert the famous hollow epidural needle into which the small flexible plastic catheter (tube), which looks like a Chinese noodle, will be threaded and through which the pain relief medication will be injected.
- 5 – They remove the epidural needle while leaving the plastic catheter in place.
- 6 – They tape the catheter along your back… and it’s done!
Does the epidural needle hurt?
Here again, it is all a matter of perspective. Everyone has their own pain tolerance. The pain that may accompany insertion of the epidural needle can also depend on when it is placed.
First, note that the prior local anesthetic is precisely intended to make the epidural needle insertion painless, or at least greatly reduce the sensation. You may feel pressure in your back that may seem strange or uncomfortable, but it normally remains completely tolerable.
You also have to take the context into account! If you were given an epidural out of the blue, when you had been feeling perfectly fine until then, then yes, it would probably be quite unpleasant. On the other hand, when it is placed while you are overwhelmed by the intensity of contractions, the experience may feel relieving rather than painful by comparison.
So the answer is: it depends! Want a little midwife’s secret? Most women say afterward that they thought getting the epidural would be much worse.
How long does an epidural last?
Rest assured: the epidural will last as long as needed.
Medical teams will take about fifteen minutes to place it, and it will take about another fifteen minutes for the effects to be felt.
Once the epidural needle is removed and the catheter is in place, as much anesthetic as needed can be administered for as long as needed! It is not a single injection that fades over time, but rather a catheter that delivers the medication on demand (continuously or intermittently, depending on the equipment).
After the epidural is stopped, its effects gradually wear off over the following hours: often 2 hours later. Depending on the situation and the woman, the effects of the epidural can last from 6 to 24 hours after childbirth.
Are there possible side effects with an epidural?
You’re going to know this answer by heart by now, but once again, it depends. Like any medical intervention, there may be certain side effects.
Keep in mind, however, that as we saw above, 80% of women in France use an epidural: it is therefore a well-established technique and procedure that would not be offered if there were major risks for you or your baby.
Some women experience side effects: some itch, others shake, some see spots before their eyes, experience drops in blood pressure, or feel nauseated…
If after an epidural you notice symptoms that bother and/or worry you, talk to the midwife caring for you; she will do everything possible to relieve that discomfort.
In other women, on the contrary, no notable side effects are observed. In that case, it is difficult, even impossible, to predict what side effects you might experience if this is your first delivery.
❗There is one specific complication risk to keep in mind: the creation of a tear in the dura mater, the membrane that surrounds the brain and spinal cord in particular. The woman then experiences severe headaches. Note, however, that in some cases the problem is easily treated with a blood patch.
Is an epidural mandatory during childbirth?
Absolutely not! An epidural is not mandatory during childbirth. Only the consultation with the anesthesiologist is, because it makes it possible to anticipate any potential complication that might require anesthesia.
However, in certain specific situations, healthcare professionals may encourage you to have one (for your safety as much as for the baby’s). For example, in cases with significant risks of a C-section or certain procedures: fetal heart rate abnormalities, twin pregnancy, breech presentation… You can still express your firm refusal.
Conversely, it is possible that you may be refused an epidural even though you want one. Contraindications are rare but far from nonexistent: certain infections, clotting disorders, use of anticoagulants, certain heart conditions, certain spinal cord or spine conditions, certain tattoos, low platelets, a back malformation, an allergy, fever… Don’t worry, further down in this article, we offer a few alternatives to an epidural.
Does an epidural have any effects on the baby?
Again, keep in mind that the risks associated with epidural anesthesia are very low. If that were not the case, it would be reserved only for high-risk deliveries. As of now, we have not identified any negative effects on the baby.
Want to learn more? Feel free to download the May app, where you’ll find plenty of resources to support and guide you throughout your pregnancy.
What alternatives are there for pain relief during childbirth?
Childbirth can absolutely take place without an epidural, whether for medical reasons or because that is the wish of the expecting mother. We have listed a few alternatives to an epidural:
- Having a midwife by your side: serious scientific studies show that the presence of a midwife by your side lowers the perception of pain. Unfortunately, nowadays in hospitals, one midwife takes care of an average of three women in labor at the same time, in addition to patients in the emergency room. It is therefore difficult for her to stay by your side continuously.
- The support of a loved one: the future co-parent can be incredibly helpful, especially if you have attended childbirth and parenting preparation sessions together. The person accompanying you can support you emotionally, massage you, help you change positions…
- Heat: it acts as a muscle relaxant and helps reduce the painful sensation of uterine contractions. You can choose a bath, a shower if you do not have access to a bathtub, or a hot water bottle placed on your lower back or stomach.
- Breathing: the uterus is a muscle, and for it to work, it needs oxygen. The problem is that when we are in pain, we tend to breathe quickly and unevenly. During labor, favor deep, full breathing and low-pitched sounds (which will relax the perineum and help you focus on something).
You can also try rectangle breathing or triangle breathing. This technique is far from working for everyone, but you have nothing to lose by trying. Ask your partner to trace a rectangle or triangle with their finger. Example with the triangle: the finger goes up = I inhale, it goes down = I exhale, it traces the bottom line = I take a short pause. The goal? To switch to autopilot, so you can detach from the pain.
- Pressure and massage: some massages and specific pressure points can reduce pain, especially when pressure is applied to the sacrum. Your partner can prepare beforehand with an independent midwife.
- Laughing gas: it works almost immediately and its effect lasts as long as you breathe it in. It is supposed to reduce pain and is widely used in pediatric emergency departments. You can inhale it throughout contractions and as much as you want.
- Positions: do not hesitate to change positions regularly to find the one that suits you best and helps reduce the pain. Just one warning: make sure your pelvis is tilted properly, never arch your back. Your back should be rounded or flat, so that your pelvis is aligned with your spine and the baby’s descent is made easier.
- Anything that can help you: in addition to all this advice, feel free to add a few personal touches that may help you de-stress, such as music, congratulating yourself at the end of each contraction, holding your partner’s hand…
France’s public health insurance covers up to 7 childbirth and parenting preparation sessions (PNP).
Also note that in cases where an epidural is contraindicated, depending on protocols and hospital practices, an IV infusion of sufentanil or a strong painkiller may also be offered.
Can the epidural needle be used outside of childbirth?
Yes, epidural anesthesia can be used for procedures other than childbirth. For an operation on the lower limbs, for example.
The idea is not to make this a “For or against epidurals?” debate, but rather to give you as much information as possible so you can make the free and informed choice that works for YOU!
Photo: BlackWhaleMedia
This text was translated from French by an artificial intelligence. The information, advice, and sources it contains comply with French standards and may therefore not apply to your situation. Make sure to complement this reading by visiting the May US/UK app and consulting the healthcare professionals who are supporting you.




