
Endometritis is one of the possible complications following childbirth. According to professors from the University of Lille, postpartum endometritis is estimated to represent 2 to 3% of postpartum infections in women. How does it present and how is it treated?
Postpartum endometritis: let’s take a closer look.
What is postpartum endometritis and what causes it?
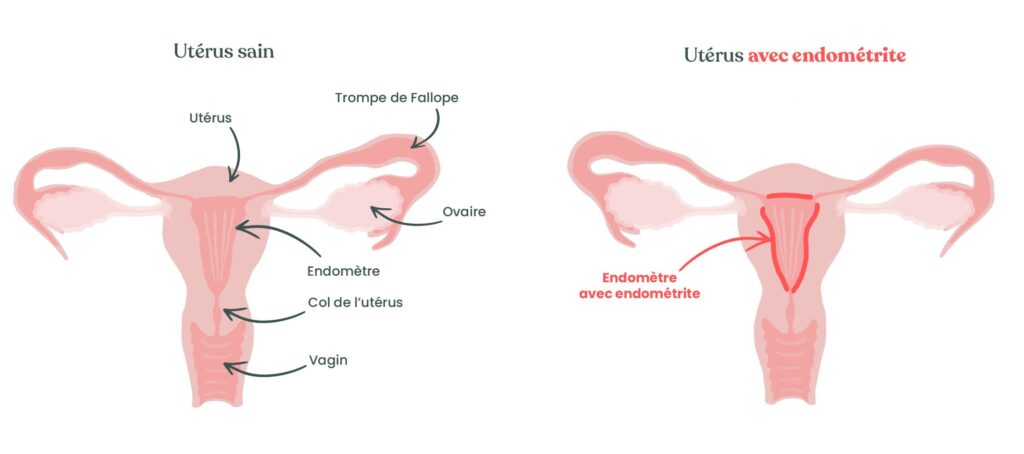
Endometritis, not to be confused with endometriosis, is an inflammation of the inner lining of the uterus, called the endometrium, caused by an infection. This condition often develops after childbirth, hence the name postpartum endometritis.
Postpartum endometritis can be caused by:
- Prolonged labor or prolonged rupture of the amniotic membranes.
- A lower genital tract infection or uterine infection already present before delivery.
- Intrauterine procedures (inside the uterus) during labor or postpartum, such as uterine revision or manual removal of the placenta (the healthcare professional inserts a hand into the uterus to remove all or part of the placenta, or to check that the uterus is empty in case of hemorrhage).
- Placental debris remaining in the uterus.
- Poor aseptic conditions during childbirth: certain obstetric or surgical procedures may also increase the risk of infection, particularly when they involve inserting instruments into the uterine cavity.
In general, healthcare professionals are careful to use sterile gynecological and obstetric equipment to avoid the risk of endometritis, whether for vaginal delivery or cesarean section. In addition, when the risk of infection is increased (intrauterine procedures, signs or risk of infection during labor), antibiotics will be administered as a preventive measure.
Outside the postpartum period, endometritis can also occur as a result of sexually transmitted infections (chlamydia, mycoplasma, etc.), tuberculosis, anemia, or following intrauterine procedures (IUD insertion, abortion, etc.).
Good to know: endometritis after childbirth occurs more often following a cesarean section, especially when it is performed as an emergency. Although childbirth can never be completely sterile, aseptic measures are systematically applied. In the case of a cesarean section, administering prophylactic antibiotics within the hour before the procedure is recommended, as it reduces the risk of endometritis by approximately 75%.
Want to learn more? Feel free to download the May app, where you’ll find plenty of resources to support and guide you throughout your pregnancy.
How to recognize postpartum endometritis and get diagnosed?
Endometritis most often presents in an acute form, but some women experience chronic endometritis. Early symptoms that appear in the days following childbirth usually include:
- Pelvic pain with uterine spasms not relieved by painkillers or local heat.
- Foul-smelling vaginal discharge.
- Fever.
- Tachycardia.
- Headaches.
- Faintness or malaise.
If you notice one or more of these symptoms, it is recommended to consult a healthcare professional. They will diagnose endometritis using a gynecological examination, which involves palpating the uterus, taking a vaginal sample (to identify the germs involved), and a blood test (to determine the stage of the infection). Additional tests may be carried out in parallel to rule out other possible causes.
Screening for chronic endometritis is strongly recommended during infertility assessments, for women who experience recurrent miscarriages or in cases of in vitro fertilization (IVF) failure.

What treatments are available for postpartum endometritis?
When treated promptly, endometritis poses no danger to the new mother. Treatment is based on antibiotics administered intravenously for at least 48 hours. The healthcare professional (gynecologist or midwife) may prescribe probiotics, as they help restore vaginal flora.
If endometritis is caused by retained placental or membrane fragments, these are removed by suction.
If left untreated, complications such as infertility, septic shock, or pelvic peritonitis (an acute inflammation of the peritoneum, the membrane lining the abdominal cavity) may occur.
Endometritis can be easily treated if diagnosed quickly. However, it is a condition that can lead to serious complications. Symptoms should not be taken lightly. Therefore, consult a healthcare professional as soon as you experience unusual symptoms after childbirth.

Postpartum medical follow-up
In general, it is important to take care of yourself after childbirth. According to the medical definition, the postpartum period lasts for about 6 to 8 weeks after birth. This duration corresponds to the time needed for the uterus to return to its pre-pregnancy size and position. However, the postpartum period varies from woman to woman and can last several months or even years.
During the first few days, you will be closely monitored, either in the maternity ward or at home, mainly by a midwife. She assesses your overall condition by examining various parameters and may call in other specialists if needed. Once you return home, follow-up can continue with a private midwife, who supports you physically and psychologically and may visit you at home several times.
During the first month, a postnatal consultation allows healthcare providers to check your overall recovery, discuss contraception, healing, breastfeeding, and any complications. Pelvic floor rehabilitation usually begins during this period. An early postnatal interview also aims to detect psychological difficulties, including postpartum depression.
In the longer term, it is important to resume regular gynecological follow-up with a midwife, gynecologist, or doctor, consider abdominal rehabilitation if necessary, and consult other healthcare professionals depending on your needs. The key is not to neglect your health and to give yourself time to fully recover.
In summary, postpartum endometritis is a relatively common infection but is generally well managed when diagnosed early. The postpartum period is a transitional, often intense time during which your body and mind need care and attention. Appropriate support, regular consultations, and careful attention to your feelings are the keys to a smooth recovery.
**
Photo credits: Dimaberlin | TrueTouchLifestyle | debbalba
This text was translated from French by an artificial intelligence. The information, advice, and sources it contains comply with French standards and may therefore not apply to your situation. Make sure to complement this reading by visiting the May US/UK app and consulting the healthcare professionals who are supporting you.




