Eczema, also known as atopic dermatitis, is a common non-contagious skin condition in babies and young children. Flare-ups most often appear as very dry skin, red patches, and itching, also called pruritus, which can sometimes be intense. How can you recognize eczema? Which creams should be used? What should you do or avoid? Eczema and atopic dermatitis in children/babies: here’s what you need to know.
How to recognize eczema in children or babies ?
Eczema appears in recurring flare-ups. These are the well-known eczema flare-ups. Over time, the condition generally progresses with periods of flare-ups alternating with remission phases. These flare-ups are often accompanied by redness and inflammatory lesions visible on your child’s skin. Its duration varies depending on the child and can last from a few months to several years. In most cases, atopic eczema gradually improves and eventually disappears during childhood. According to French Health Insurance, atopic dermatitis persists into adulthood in only 5% of cases. Symptoms to watch for in your child:
- Skin that is so dry it becomes rough (you feel it more than you see it).
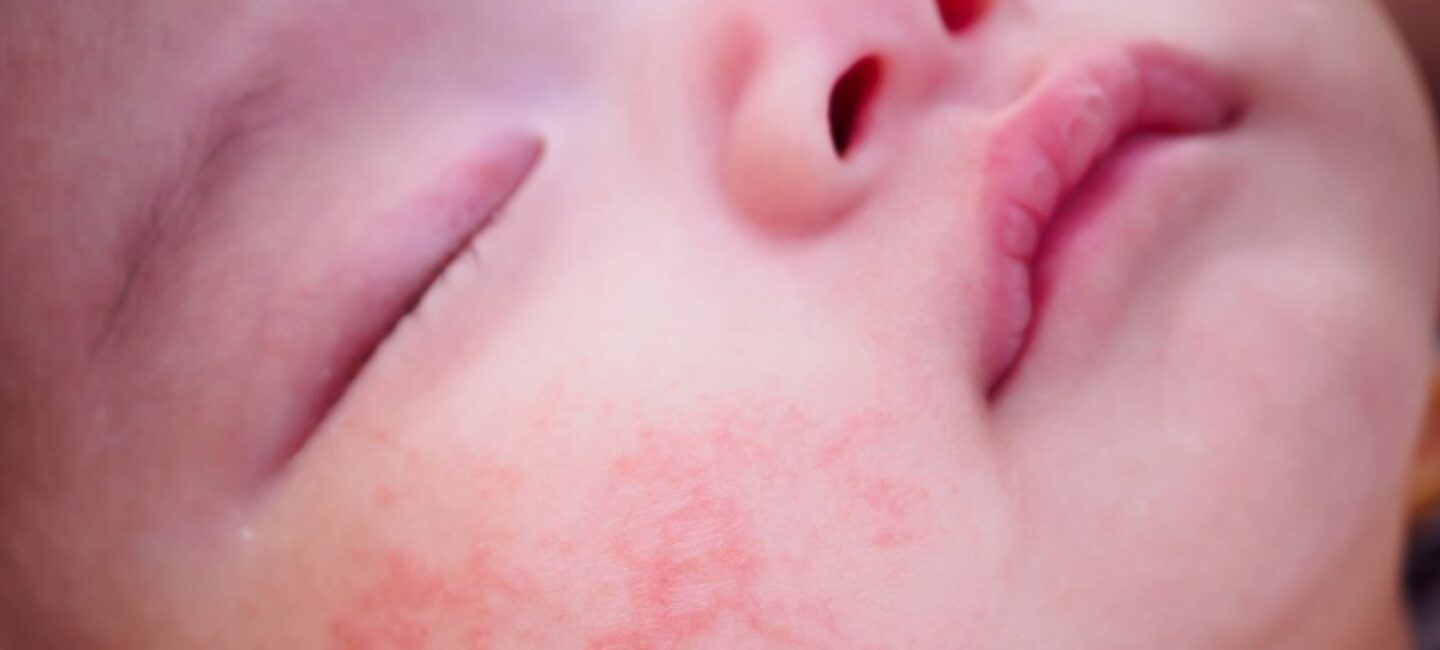
- Red patches especially on the face, trunk, and in skin folds.
- Your child tries to scratch day and night.
In this case, there’s little doubt—it’s likely eczema. A diagnosis by a doctor is still necessary. Make an appointment with your pediatrician to confirm the diagnosis. In case of severe or persistent symptoms, a consultation with a dermatologist may also be recommended. Good to know: atopic eczema is often hereditary. According to French Health Insurance, in 50 to 70% of cases, a first-degree relative has already had it. Want to learn more? Feel free to download the May app, where you’ll find plenty of resources to support and guide you throughout your journey as a new parent. 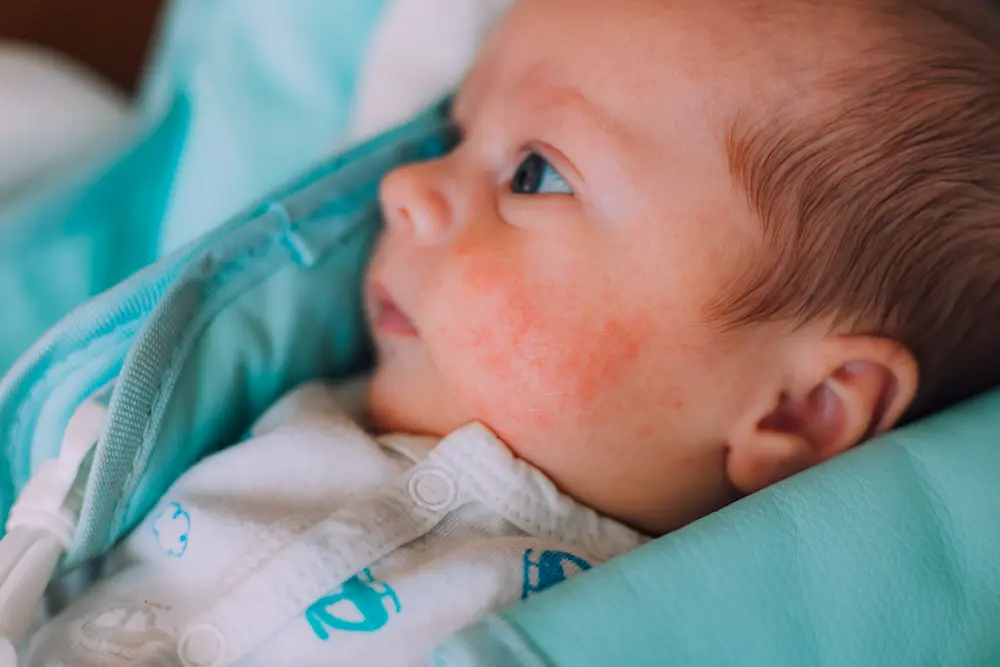
Where does eczema develop on a child’s body depending on age?
Atopic eczema in children can present differently depending on age. The location of lesions, their appearance, and the affected areas of the body evolve over time.
Eczema in babies between 0 and 1 year
In babies aged 0 to 1 year, infant eczema usually appears symmetrically. Lesions mainly affect the convex areas of the face (forehead, cheeks, chin) as well as certain parts of the limbs such as arms and legs. However, the nose and buttocks are usually spared. The folds behind and under the ears may show cracks and oozing, while the front neck fold is also often affected. Good to know: if small greasy white or yellowish patches appear on your baby’s scalp, they are probably cradle cap.
Eczema in children aged 1 to 2 years
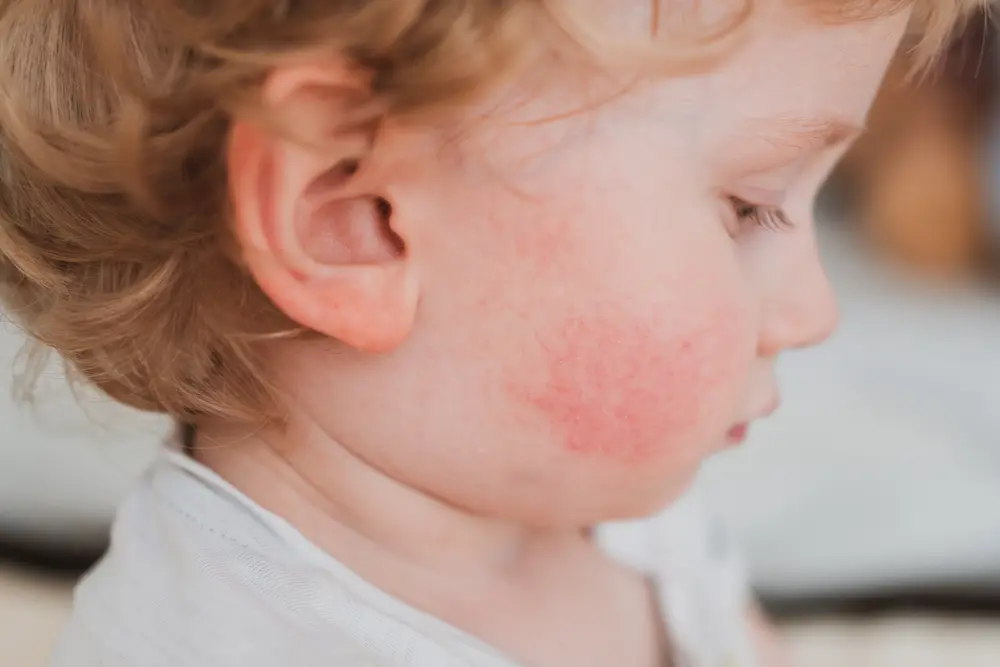
Between 1 and 2 years, atopic eczema appears mainly on the head, neck, and flexural folds. Lesions may also appear on the trunk and limbs, forming round red patches about the size of a coin. In general, the palms, soles of the feet, and nose are rarely affected.
Eczema in children over 2 years old
After age 2, atopic eczema lesions often become thicker and whitish, with a lichenified appearance, causing significant itching. The face is less frequently affected, but the area under the lower eyelids may appear darker, thicker, and marked by pronounced folds. The area around the mouth may also be affected. Lesions are mainly located in skin folds (neck, behind the ears, elbows, knees), but also on the hands, wrists, and ankles. More rarely, they may extend to other parts of the limbs. The skin is generally very dry, especially on the hands, where it may become cracked or fissured. 
What to do in case of eczema and atopic dermatitis in children or babies?
Treatments to relieve eczema in babies and children exist and are highly effective.
Which cream should be used to treat eczema and atopic dermatitis in children or babies?
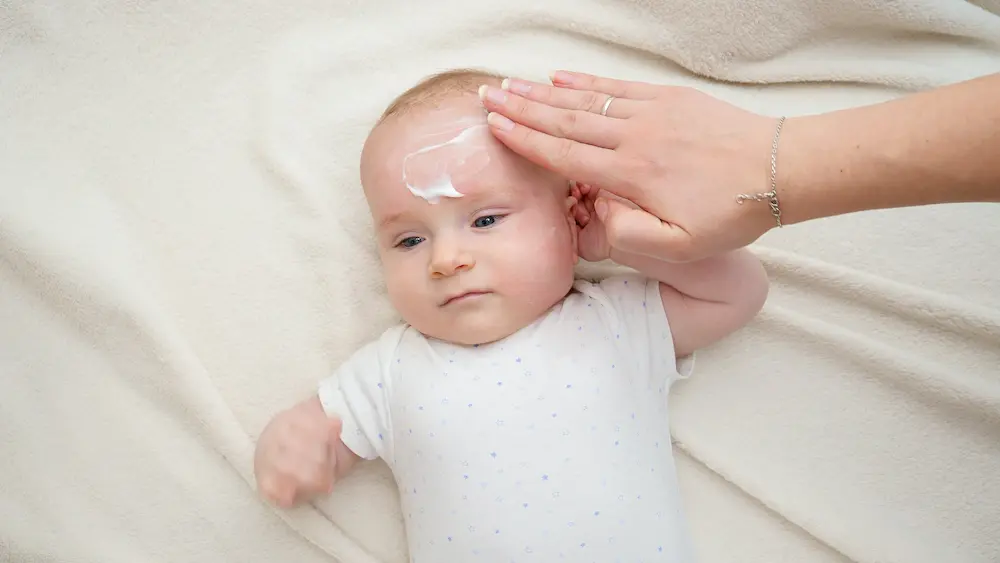
Good hydration helps limit dryness and protect the skin from irritation. Here’s how to proceed: Wash your child with a syndet (“soap-free”) fragrance-free cleanser that won’t further dry out the skin. Rinse thoroughly. Use an emollient cream without fragrance, preferably in balm form such as Exomega Balm® or Xémose Balm®. You can apply this balm twice a day. Apply it preferably after bathing as it will penetrate the skin better, since the pores are more open. Emollient treatment is the foundation of eczema care in babies. It helps space out flare-ups and may even protect against the development of allergies by restoring the skin’s barrier function.
Eczema and atopic dermatitis in children or babies: topical corticosteroids
These are cortisone-based creams that treat your child’s skin and help eczema disappear. They should be applied once a day to affected areas until symptoms completely disappear. Warning: usually a different cream is used for the face and the body. For the body, doctors tend to prescribe a stronger corticosteroid, while for the face a milder, moderate-strength cream is used. Many parents are afraid of cortisone creams and apply them too sparingly. In reality, the skin is more damaged by eczema than by topical corticosteroids, which are essential for healing your baby’s eczema.
Other care to treat eczema and atopic dermatitis in children or babies
- Short baths (max 10 minutes) or showers. Bath water should be lukewarm (max 33°C). You can wash your child every other day—no need to dry out their skin further.
- No vigorous rubbing when drying your child after bathing. Pat gently with a soft towel.
- Use cotton underwear. Avoid pressure points and buttons in direct contact with your child’s skin.
- Keep nails short and as clean as possible to prevent infections.
- No contact with people who have herpes (cold sores), as this may cause a secondary infection in your child.
- Make sure to ventilate the bedroom well and maintain a moderate temperature (19°C).
- Limit your child’s exposure to allergens or irritants as much as possible, such as dust, pets, perfumes and scented fabric softeners, wool, synthetic fabrics, cigarette smoke, urban industrial pollution, dry cold air, and humid heat (sweating worsens lesions).
- Rinse thoroughly with fresh water after swimming pool baths, as chlorine is harsh on the skin.
What to avoid in case of eczema and atopic dermatitis in children or babies
- Scratchy clothing can worsen itching. Avoid materials like wool and choose soft cotton.
- Do not use skincare products containing sweet almond oil, wheat, or oats (except purified Rhealba oat plantlets without proteins), sesame, or other food-based ingredients. Not only do oils not properly hydrate, but these products may later cause food allergies, especially to nuts.
Warning signs in case of eczema and atopic dermatitis in children or babies
Eczema can lead to more serious skin infections such as impetigo. These are usually bacterial infections. Consult your pediatrician quickly if your child does not respond to standard treatments or shows one of the following symptoms:
- the appearance of fever during flare-ups,
- a change in usual lesions (oozing, crusting, pus-filled bumps, or even an unpleasant odor).
Does my child have “atopy” and/or a food allergy?
Atopy is a genetic predisposition to develop “allergic” diseases such as eczema (also called atopic dermatitis), asthma, respiratory allergies (such as hay fever or dust mite allergic rhinitis), and food allergies. If your child has eczema, they are at higher risk than other children of developing one of these conditions. But that does not necessarily mean they have a food allergy! Food allergy tests are only performed if eczema does not respond to well-managed treatment or if it is accompanied by other symptoms suggestive of a food allergy. In summary, eczema is a common condition in babies and children, characterized by flare-ups of red patches, very dry skin, and significant itching. Fortunately, proper skin hydration and effective treatment generally help relieve your child and control flare-ups. ** Photo credits: aliona2194 | ta_bu | kryzhov | natalyaraeva This text was translated from French by an artificial intelligence. The information, advice, and sources it contains comply with French standards and may therefore not apply to your situation. Make sure to complement this reading by visiting the May US/UK app and consulting the healthcare professionals who are supporting you.